When you’re managing a chronic condition like high blood pressure or type 2 diabetes, your doctor might prescribe a combo generic - a single pill that combines two or more medications. It sounds convenient, right? Fewer pills to remember, fewer trips to the pharmacy. But here’s the catch: that convenience often comes at a steep price. In many cases, buying the same drugs as separate generic components saves you hundreds - sometimes thousands - of dollars a year.
Why Combo Pills Cost So Much
Fixed-dose combinations (FDCs) are marketed as a one-stop solution. But behind the scenes, pharmaceutical companies use them to extend patent life and maintain high prices. A 2018 study from Boston University, published in JAMA Internal Medicine, found that Medicare Part D spent $925 million more in 2016 on 29 branded combo drugs than it would have if patients had been prescribed the same drugs as individual generics. That’s not a rounding error - that’s nearly a billion dollars in avoidable spending. Take Janumet, a combo of sitagliptin and metformin. In 2016, Medicare paid an average of $472 for a 30-day supply of the branded version. Meanwhile, generic metformin alone cost as little as $4 for the same duration at Walmart’s $4 program. Even if you added the cost of the sitagliptin component (which was still under patent), you’d still be paying far less than the combo pill. This pattern repeats across dozens of popular FDCs - Kazano, Entresto, Synjardy - where one component is generic and the other is brand-name, yet the combo is priced as if both are new and expensive. The math doesn’t add up. IQVIA’s 2022 analysis showed that branded FDCs typically cost 60% of what two separate branded drugs would cost. But when one or both components are available as generics? The combo often costs 10 to 15 times more than buying them separately. This isn’t innovation - it’s a pricing loophole.How Generic Competition Drives Down Prices
Generic drugs don’t just save money - they transform markets. Once a brand-name drug loses exclusivity, prices drop fast. With three generic competitors, prices fall about 20%. With 10 or more, they plummet 70-80%. The FDA reports that generics cost, on average, 80-85% less than their brand-name counterparts. So why do combo pills resist this trend? The answer lies in how they’re structured. If a combo pill includes one drug that’s still under patent - say, bempedoic acid in Nexlizet - the manufacturer can price the whole thing like a new drug, even though the other component (ezetimibe) has been generic for years. In Europe, Nexlizet costs around €5 per day. In the U.S., it’s $12 per day. But ezetimibe alone? You can get it for less than $10 a month. That’s not a premium for convenience - it’s a premium for exploiting the system. A 2020 report from the U.S. Department of Health and Human Services showed that 90.2% of all prescriptions in 2019 were filled as generics. Yet combo drugs are an exception. Between 2015 and 2020, their use grew by 14.7% annually. Meanwhile, they made up only 2.1% of all prescriptions but accounted for 8.3% of Medicare Part D spending in 2021. In other words, a tiny fraction of prescriptions was soaking up nearly one-tenth of the budget.Real-World Cost Differences You Can See Today
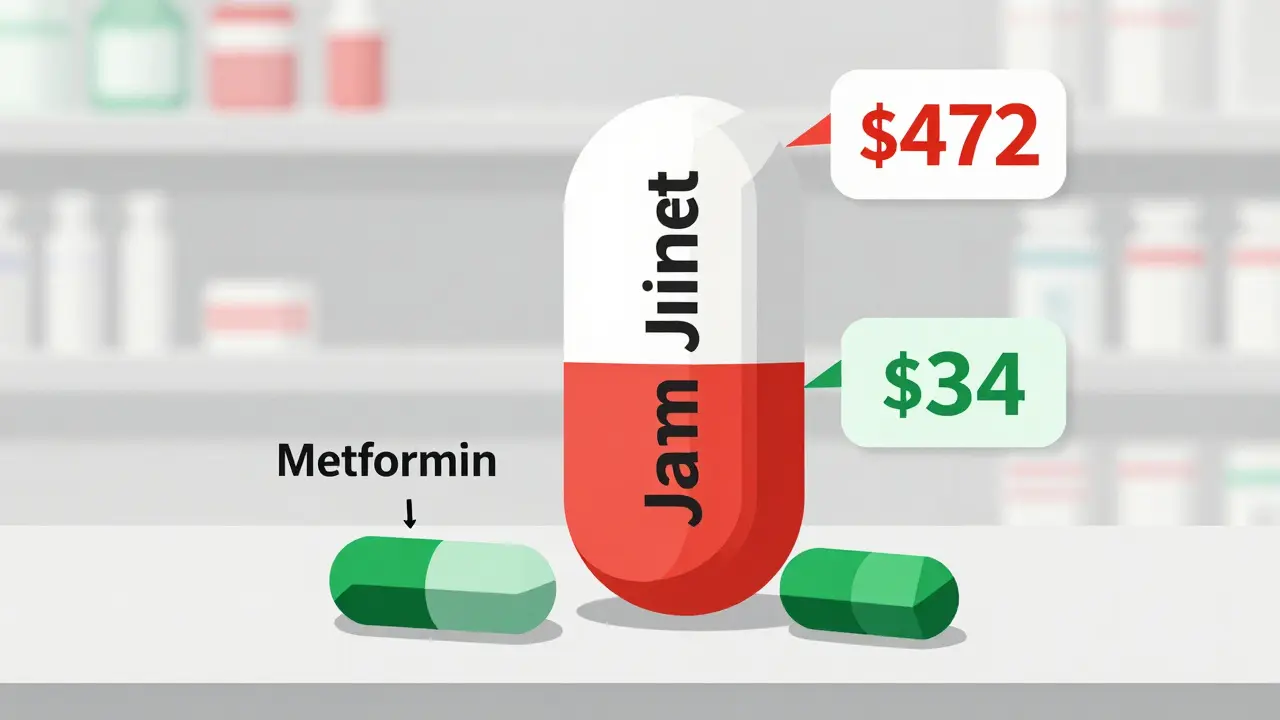
Let’s break down a few real examples - all based on 2023 pricing in the U.S.:- Janumet (sitagliptin + metformin): Branded FDC costs $472/month. Generic metformin: $4/month. Generic sitagliptin (available since 2022): $30/month. Total for separate generics: $34/month. Savings: $438/month, or over $5,200 a year.
- Kazano (alogliptin + metformin): Branded FDC: $425/month. Generic metformin: $4/month. Generic alogliptin: $55/month. Total for generics: $59/month. Savings: $366/month, or $4,392/year.
- Entresto (sacubitril + valsartan): Branded FDC: $550/month. Generic valsartan: $12/month. Sacubitril (still under patent): $280/month. Total for separate drugs: $292/month. Savings: $258/month, or $3,096/year.

Why Doctors Still Prescribe Combos
You might wonder: if the savings are this clear, why don’t more doctors skip the combo? The answer is layered. First, many prescribers aren’t aware of the price gap. Pharmacy systems often default to the combo pill because it’s listed as the primary option in electronic prescribing tools. Second, there’s a belief that fewer pills = better adherence. Studies do show that patients on combo pills are 15-20% more likely to stick to their regimen than those taking multiple pills. But here’s the twist: adherence doesn’t have to cost $500 a month. A 2020 case study from the University of Michigan Health System found that when pharmacists proactively switched patients from branded combos to separate generics - with clear counseling and pill organizers - adherence stayed the same. In fact, patients reported feeling more in control of their care. The real barrier isn’t patient behavior - it’s system inertia.What You Can Do to Save Money
If you’re on a combo drug, here’s what to ask your pharmacist or doctor:- Are both components available as generics? Use a tool like GoodRx or RxSaver to compare prices. If one is generic and the other isn’t, ask if you can get the brand-name component alone and pair it with the generic.
- Can you split the combo? Some pharmacies will fill a prescription for two separate generics and package them together as a blister pack - no extra cost.
- Ask about prior authorization. Many Medicare Part D plans require it for expensive combos. If your plan denies coverage, they’ll often approve the cheaper generic alternative.
- Check your plan’s formulary. Some plans have a “preferred generic” policy that gives you a $0 or $5 co-pay for separate components, while the combo is placed in a higher tier.
The Bigger Picture: Policy and Reform
The Inflation Reduction Act of 2022 gave Medicare the power to negotiate drug prices - and combo drugs are high on the list. The Congressional Budget Office estimates that if current trends continue, Medicare will spend an extra $14.3 billion on branded combos over the next decade. That’s money that could go toward insulin, cancer drugs, or mental health care. The FDA is also speeding up generic approvals. With more components hitting the market as generics, the pricing gap will only widen. Meanwhile, manufacturers are trying to keep up with programs like Novartis’s $10 co-pay offer for Entresto. But even that’s still 10 times the cost of the generic alternative.Bottom Line: Convenience Isn’t Worth the Cost
Combo pills aren’t evil. They’re useful in some cases - especially for patients with complex regimens or cognitive challenges. But for most people, they’re a financial trap. The idea that convenience justifies a 10x price jump doesn’t hold up under scrutiny. You’re not paying for innovation. You’re paying for a loophole. The data is clear: if your combo drug includes one or more generic components, you’re almost certainly overpaying. Talk to your pharmacist. Run the numbers. Ask for alternatives. You could save thousands - and still take the exact same medicines.Are combo generics always more expensive than buying individual generics?
Not always - but in the vast majority of cases, yes. If one or both components of a combo pill are available as generics, buying them separately almost always costs less. The only exceptions are when both components are still under patent and no generics exist. But even then, the combo is rarely cheaper than the sum of two separate brand-name drugs. Most combo drugs on the market today contain at least one generic ingredient, making them overpriced by design.
Can I ask my doctor to switch me from a combo pill to separate generics?
Absolutely. Doctors are required to prescribe based on medical need and cost-effectiveness. If you’re paying $500 a month for a combo pill when the same drugs cost $50 as generics, your doctor should consider the switch. Bring a price comparison from GoodRx or your pharmacy - many prescribers are unaware of the cost gap. Most patients who switch report no change in effectiveness and a big drop in out-of-pocket costs.
Why don’t pharmacies automatically offer the cheaper option?
Pharmacies often follow default prescribing patterns set by electronic health record systems and insurance formularies. If the combo pill is listed as the primary option, it’s what gets filled unless someone specifically requests otherwise. Pharmacists can help - but you need to ask. Don’t assume they’ll catch it. Always check your receipt and compare prices before leaving the pharmacy.
Does taking separate pills hurt adherence?
Not necessarily. Studies show that adherence improves with combo pills - but only if the pills are simple to manage. When patients are given clear instructions, pill organizers, or blister packs with separate generics, adherence stays just as high. The real issue isn’t the number of pills - it’s whether patients understand how to take them. Many people do better with two pills they can track than one confusing combo.
What should I do if my insurance won’t cover the separate generics?
Ask your pharmacist to file a prior authorization or exception request. Many insurance plans will cover the generics if you prove the combo is significantly more expensive. You can also use patient assistance programs - some manufacturers offer free or discounted generics if you qualify. And don’t forget: you can always pay cash. At pharmacies like Walmart, Target, or Costco, generic versions of common combo drugs can cost less than $10 for a 30-day supply.

becca roberts
So let me get this straight - we’re paying $500/month for a pill that’s literally just two generics glued together, and the system calls this "innovation"? 😑
Pharma’s playing chess while we’re stuck playing checkers with our insulin pens.